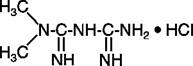These highlights do not include all the information needed to use METFORMIN HYDROCHLORIDE EXTENDED-RELEASE
TABLETS safely and effectively. See full prescribing information for METFORMIN HYDROCHLORIDE EXTENDED-RELEASE TABLETS. METFORMIN HYDROCHLORIDE extended-release tablets, for oral useInitial U.S. Approval: 1995 · Nostrum Laboratories, Inc.
Postmarketing cases of metformin-associated lactic acidosis have resulted in death, hypothermia, hypotension, and resistant bradyarrhythmias. The onset of metformin- associated lactic acidosis is often subtle, accompanied only by nonspecific symptoms such as malaise, myalgias, respiratory distress, somnolence, and abdominal pain. Metformin- associated lactic acidosis was characterized by elevated blood lactate levels (>5 mmol/Liter), anion gap acidosis (without evidence of ketonuria or ketonemia), an increased lactate/pyruvate ratio; and metformin plasma levels generally >5 mcg/mL [see Warnings and Precautions (5.1)].
Risk factors for metformin-associated lactic acidosis include renal impairment, concomitant use of certain drugs (e.g. carbonic anhydrase inhibitors such as topiramate), age 65 years old or greater, having a radiological study with contrast, surgery and other procedures, hypoxic states (e.g., acute congestive heart failure), excessive alcohol intake, and hepatic impairment.
Steps to reduce the risk of and manage metformin-associated lactic acidosis in these high risk groups are provided [see Dosage and Administration (2.2), Contraindications (4), Warnings and Precautions (5.1)].
If metformin-associated lactic acidosis is suspected, immediately discontinue Metformin hydrochloride extended-release tablets and institute general supportive measures in a hospital setting. Prompt hemodialysis is recommended [see Warnings and Precautions (5.1)].
Metformin hydrochloride extended-release tablets are indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
Metformin hydrochloride extended-release tablets, USP are available as:
- 500 mg extended-release, white to off-white, film coated, modified capsule-shaped tablets debossed with “NF5” on one side.
- 1,000 mg extended-release, white to off-white, film coated, modified capsule-shaped tablets debossed with “NF0” on one side.
Metformin hydrochloride extended-release tablets are contraindicated in patients with:
- Severe renal impairment (eGFR below 30 mL/min/1.73 m2) [see Warnings and Precautions (5.1) ].
- Hypersensitivity to metformin.
- Acute or chronic metabolic acidosis, including diabetic ketoacidosis, with or without coma.
Table 2 presents clinically significant drug interactions with Metformin hydrochloride extended-release tablets.
|
Carbonic Anhydrase Inhibitors
|
|
|
Clinical Impact:
|
Carbonic anhydrase inhibitors frequently cause a decrease in serum bicarbonate and induce non-anion gap, hyperchloremic metabolic acidosis. Concomitant use of these drugs with Metformin hydrochloride extended-release tablets may increase the risk for lactic acidosis. |
|
Intervention:
|
Consider more frequent monitoring of these patients. |
|
Examples:
|
Topiramate, zonisamide, acetazolamide or dichlorphenamide. |
|
Drugs that Reduce Metformin hydrochloride hxtended-release tablets Clearance
|
|
|
Clinical Impact:
|
Concomitant use of drugs that interfere with common renal tubular transport systems involved in the renal elimination of metformin (e.g., organic cationic transporter-2 [OCT2] / multidrug and toxin extrusion [MATE] inhibitors) could increase systemic exposure to metformin and may increase the risk for lactic acidosis [see Clinical Pharmacology (12.3)].
|
|
Intervention:
|
Consider the benefits and risks of concomitant use with Metformin hydrochloride extended-release tablets. |
|
Examples:
|
Ranolazine, vandetanib, dolutegravir, and cimetidine. |
|
Alcohol
|
|
|
Clinical Impact:
|
Alcohol is known to potentiate the effect of metformin on lactate metabolism. |
|
Intervention:
|
Warn patients against excessive alcohol intake while receiving Metformin hydrochloride extended-release tablets. |
|
Insulin Secretagogues or Insulin
|
|
|
Clinical Impact:
|
Coadministration of Metformin hydrochloride extended-release tablets with an insulin secretagogue (e.g., sulfonylurea) or insulin may increase the risk of hypoglycemia. |
|
Intervention:
|
Patients receiving an insulin secretagogue or insulin may require lower doses of the insulin secretagogue or insulin. |
|
Drugs Affecting Glycemic Control
|
|
|
Clinical Impact:
|
Certain drugs tend to produce hyperglycemia and may lead to loss of glycemic control. |
|
Intervention:
|
When such drugs are administered to a patient receiving Metformin hydrochloride extended-release tablets, observe the patient closely for loss of blood glucose control. When such drugs are withdrawn from a patient receiving Metformin hydrochloride extended-release tablets, observe the patient closely for hypoglycemia. |
|
Examples:
|
Thiazides and other diuretics, corticosteroids, phenothiazines, thyroid products, estrogens, oral contraceptives, phenytoin, nicotinic acid, sympathomimetics, calcium channel blockers, and isoniazid. |
Risk Summary
Limited data with Metformin hydrochloride extended-release tablets in pregnant women are not sufficient to determine a drug-associated risk for major birth defects or miscarriage. Published studies with metformin use during pregnancy have not reported a clear association with metformin and major birth defect or miscarriage risk [see Data]. There are risks to the mother and fetus associated with poorly controlled diabetes mellitus in pregnancy [see Clinical Considerations].
No adverse developmental effects were observed when metformin was administered to pregnant Sprague Dawley rats and rabbits during the period of organogenesis at doses up to 2- and 5- times, respectively, a 2550 mg clinical dose, based on body surface area [see Data].
The estimated background risk of major birth defects is 6 to 10% in women with pre-gestational diabetes mellitus with an HbA1C >7 and has been reported to be as high as 20 to 25% in women with a HbA1C >10. The estimated background risk of miscarriage for the indicated population is unknown. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2 to 4% and 15 to 20%, respectively.
Clinical Considerations
Disease-associated maternal and/or embryo/fetal risk:
Poorly-controlled diabetes mellitus in pregnancy increases the maternal risk for diabetic ketoacidosis, pre-eclampsia, spontaneous abortions, preterm delivery, stillbirth and delivery complications. Poorly controlled diabetes mellitus increases the fetal risk for major birth defects, stillbirth, and macrosomia related morbidity.
Data
Human Data:
Published data from post-marketing studies have not reported a clear association with metformin and major birth defects, miscarriage, or adverse maternal or fetal outcomes when metformin was used during pregnancy. However, these studies cannot definitely establish the absence of any metformin-associated risk because of methodological limitations, including small sample size and inconsistent comparator groups.
Animal Data:
Metformin HCl did not adversely affect development outcomes when administered to pregnant rats and rabbits at doses up to 600 mg/kg/day. This represents an exposure of about 2 and 5 times a 2550 mg clinical dose based on body surface area comparisons for rats and rabbits, respectively. Determination of fetal concentrations demonstrated a partial placental barrier to metformin.
Safety and effectiveness of Metformin hydrochloride extended-release tablets in pediatric patients have not been established.
Controlled clinical studies of Metformin hydrochloride extended-release tablets did not include sufficient numbers of elderly patients to determine whether they respond differently from younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy and the higher risk of lactic acidosis. Assess renal function more frequently in elderly patients [see Warnings and Precautions (5.1)].
Overdose of metformin HCl has occurred, including ingestion of amounts greater than 50 grams. Hypoglycemia was reported in approximately 10% of cases, but no causal association with metformin has been established. Lactic acidosis has been reported in approximately 32% of metformin overdose cases [see Warnings and Precautions (5.1)]. Metformin is dialyzable with a clearance of up to 170 mL/min under good hemodynamic conditions. Therefore, hemodialysis may be useful for removal of accumulated drug from patients in whom metformin overdosage is suspected.
Advise the patient to read the FDA-approved patient labeling (Patient Information).
Lactic Acidosis
Explain the risks of lactic acidosis, its symptoms, and conditions that predispose to its development. Advise patients to discontinue Metformin hydrochloride extended-release tablets immediately and to promptly notify their healthcare provider if unexplained hyperventilation, myalgias, malaise, unusual somnolence or other nonspecific symptoms occur. Counsel patients against excessive alcohol intake and inform patients about importance of regular testing of renal function while receiving Metformin hydrochloride extended-release tablets. Instruct patients to inform their doctor that they are taking Metformin hydrochloride extended-release tablets prior to any surgical or radiological procedure, as temporary discontinuation may be required [see Warnings and Precautions (5.1)].
Hypoglycemia
Inform patients that hypoglycemia may occur when Metformin hydrochloride extended-release tablets are coadministered with oral sulfonylureas and insulin. Explain to patients receiving concomitant therapy the risks of hypoglycemia, its symptoms and treatment, and conditions that predispose to its development [see Warnings and Precautions (5.3)].
Vitamin B12 Deficiency
Inform patients about importance of regular hematological parameters while receiving Metformin hydrochloride extended-release tablets [see Warnings and Precautions (5.2)].
Females of Reproductive Age
Inform females that treatment with Metformin hydrochloride extended-release tablets may result in ovulation in some premenopausal anovulatory women which may lead to unintended pregnancy [see Use in Specific Populations (8.3)].
Administration Information
Inform patients that Metformin hydrochloride extended-release tablets must be swallowed whole and not crushed, cut, or chewed, and that the inactive ingredients may occasionally be eliminated in the feces as a soft mass that may resemble the original tablet.
Manufactured by:
Nostrum Laboratories, Inc
Kansas City, MO 64120
Rev. January 2019
Metformin hydrochloride extended-release tablets, USP contain the biguanidine antihyperglycemic agent, metformin, in the form of monohydrochloride salt. The chemical name of metformin HCl is N, N-dimethylimidodicarbonimidic diamide hydrochloride with a molecular formula of C4H11N5•HCl and a molecular weight of 165.63. Its structural formula is:
[image: MM1]Metformin HCl is a white to off-white crystalline powder that is freely soluble in water and is practically insoluble in acetone, ether, and chloroform. The pKa of metformin is 12.4. The pH of a 1% aqueous solution of metformin HCl is 6.68.
Metformin hydrochloride extended-release tablets, USP deliver 500 mg or 1,000 mg of metformin HCl, which is equivalent to 389.93 mg or 779.86 mg metformin, respectively. In addition to the active ingredient metformin HCl, each tablet contains the following inactive ingredients: ammonium hydroxide, ethylcellulose, hypromellose, lactose monohydrate, medium chain triglycerides, oleic acid, polyethylene glycol, povidone, silicified microcrystalline cellulose, stearic acid, titanium dioxide, talc, triacetin and xanthan gum.
USP dissolution test is pending
NDC 29033-031-06
Metformin Hydrochloride Extended-release Tablets, USP
500 mg
Rx only
60 Tablets
[image: MM2]
NDC 29033-032-06
Metformin Hydrochloride Extended-release Tablets, USP
1000 mg
Rx only
60 Tablets
[image: MM3]
Metformin hydrochloride extended-release tablets, USP as are supplied as modified capsule-shaped, film-coated extended-release tablets containing 500 mg or 1,000 mg of metformin hydrochloride.
NDC 29033-031-06: 500 mg extended-release, white to off-white, film coated, modified capsule-shaped tablets debossed with “NF5” on one side: bottles of 60.
NDC 29033-032-06: 1,000 mg extended-release, white to off-white, film coated, modified capsule-shaped tablets debossed with “NF0” on one side: bottles of 60.
What it looks like
Photos of the product and/or packaging supplied by the manufacturer.
Package codes (NDC)
- 29033-031-06
- 29033-032-06
Full prescribing information (for healthcare professionals)
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Metformin is an antihyperglycemic agent which improves glucose tolerance in patients with type 2 diabetes mellitus, lowering both basal and postprandial plasma glucose. Metformin decreases hepatic glucose production, decreases intestinal absorption of glucose, and improves insulin sensitivity by increasing peripheral glucose uptake and utilization. With metformin therapy, insulin secretion remains unchanged while fasting insulin levels and day-long plasma insulin response may decrease.
12.3 Pharmacokinetics
Absorption
In a multiple-dose crossover study, 23 patients with type 2 diabetes mellitus were administered either Metformin hydrochloride extended-release tablets 2,000 mg once a day (after dinner) or metformin HCl tablets 1,000 mg twice a day (after breakfast and after dinner). After 4 weeks of treatment, steady-state pharmacokinetic parameters, area under the concentration-time curve (AUC), time to peak plasma concentration (Tmax), and maximum concentration (Cmax) were evaluated. The appearance of metformin in plasma from Metformin hydrochloride extended-release tablets are slower and more prolonged compared to metformin HCl tablets. Results are presented in Table 3.
|
Pharmacokinetic
Parameters (mean ± SD) |
Metformin hydrochloride extended-release tablets
2,000 mg (administered q.d. after dinner) |
Metformin HCl tablets
2,000 mg (1,000 mg b.i.d.) |
| AUC0-24hr (ng•hr/mL) |
26,811 ± 7055 |
27,371 ± 5,781 |
| Tmax (hr) |
6 (3 to 10) |
3 (1 to 8) |
| Cmax (ng/mL) |
2849 ± 797 |
1820 ± 370 |
In four single-dose studies and one multiple-dose study, the bioavailability of Metformin hydrochloride extended-release tablets 2,000 mg given once daily, in the evening, under fed conditions [as measured by AUC] was similar to the same total daily dose administered as metformin HCl tablets 1,000 mg given twice daily. The geometric mean ratios (Metformin hydrochloride extended-release tablets / metformin HCL tablets) of AUC0-24hr, AUC0-72hr, and AUC0-inf for these five studies ranged from 0.96 to 1.08.
In a single-dose, four-period replicate crossover design study, comparing two 500 mg Metformin hydrochloride extended-release tablets to one 1,000 mg Metformin hydrochloride extended-release tablet administered in the evening with food to 29 healthy male subjects, two 500 mg Metformin hydrochloride extended-release tablets were found to be equivalent to one 1,000 mg Metformin hydrochloride extended-release tablet.
In a study carried out with Metformin hydrochloride extended-release tablets, there was a dose-associated increase in metformin exposure over 24 hours following oral administration of 1,000, 1,500, 2,000, and 2,500 mg.
In three studies with Metformin hydrochloride extended-release tablets using different treatment regimens (2,000 mg after dinner; 1,000 mg after breakfast and after dinner; and 2,500 mg after dinner), the pharmacokinetics of metformin as measured by AUC appeared linear following multiple-dose administration.
Effect of food: The extent of metformin absorption (as measured by AUC) from Metformin hydrochloride extended-release tablets increased by approximately 60% when given with food. When Metformin hydrochloride extended-release tablets was administered with food, Cmax was increased by approximately 30% and Tmax was more prolonged compared with the fasting state (6.1 versus 4.0 hours).
Distribution
The apparent volume of distribution (V/F) of metformin following single oral doses of metformin HCl tablets 850 mg averaged 654 ± 358 L. Metformin is negligibly bound to plasma proteins. Metformin partitions into erythrocytes, most likely as a function of time.
Metabolism
Intravenous single-dose studies in normal subjects demonstrate that metformin is excreted unchanged in the urine and does not undergo hepatic metabolism (no metabolites have been identified in humans) nor biliary excretion.
Elimination
Renal clearance (see Table 4) is approximately 3.5 times greater than creatinine clearance, which indicates that tubular secretion is the major route of metformin elimination. Following oral administration, approximately 90% of the absorbed drug is eliminated via the renal route within the first 24 hours, with a plasma elimination half-life of approximately 6.2 hours. In blood, the elimination half-life is approximately 17.6 hours, suggesting that the erythrocyte mass may be a compartment of distribution.
Specific Populations
Renal Impairment:
In patients with decreased renal function the plasma and blood half-life of metformin is prolonged and the renal clearance is decreased (see Table 4) [See Dosage and Administration (2.2), Contraindications (4), and Warnings and Precautions (5.1) and Use in Specific Populations (8.6)].
Hepatic Impairment:
No pharmacokinetic studies of metformin have been conducted in patients with hepatic impairment [See Warnings and Precautions (5.1) and Use in Specific Populations (8.7)].
Geriatrics:
Limited data from controlled pharmacokinetic studies of metformin HCl tablets in healthy elderly subjects suggest that total plasma clearance of metformin is decreased, the half-life is prolonged, and Cmax is increased, compared to healthy young subjects. It appears that the change in metformin pharmacokinetics with aging is primarily accounted for by a change in renal function (see Table 4). [See Warnings and Precautions (5.1) and Use in Specific Populations (8.5)].
|
Subject Groups: Metformin HCl dosea
(number of subjects) |
Cmax
b
(mcg/mL) |
Tmax
c
(hrs) |
Renal Clearance (mL/min)
|
|
Healthy, nondiabetic adults:
500 mg single dose (24) 850 mg single dose (74)d 850 mg three times daily for 19 dosese (9) |
1.03 (±0.33) 1.60 (±0.38) 2.01 (±0.42) |
2.75 (±0.81) 2.64 (±0.82) 1.79 (±0.94) |
600 (±132) 552 (±139) 642 (±173) |
|
Adults with type 2 diabetes mellitus:
850 mg single dose (23) 850 mg three times daily for 19 dosese (9) |
1.48 (±0.5) 1.90 (±0.62) |
3.32 (±1.08) 2.01 (±1.22) |
491 (±138) 550 (±160 |
|
Elderlyf, healthy nondiabetic adults:
850 mg single dose (12) |
2.45 (±0.70) |
2.71 (±1.05) |
412 (±98) |
|
Renal-impaired adults:
850 mg single dose Mild (CLcrg 61 to 90 mL/min) (5) Moderate (CLcr 31 to 60 mL/min) (4) Severe (CLcr 10 to 30 mL/min) (6) |
1.86 (±0.52) 4.12 (±1.83) 3.93 (±0.92) |
3.20 (±0.45) 3.75 (±0.50) 4.01 (±1.10) |
384 (±122) 108 (±57) 130 (±90) |
a All doses given fasting except the first 18 doses of the multiple dose studies
b Peak plasma concentration
c Time to peak plasma concentration
d Combined results (average means) of five studies: mean age 32 years (range 23 to 59 years)
e Kinetic study done following dose 19, given fasting
f Elderly subjects, mean age 71 years (range 65 to 81 years)
g CLcr = creatinine clearance normalized to body surface area of 1.73 m2
Pediatrics:
There are no available pharmacokinetic data with Metformin hydrochloride extended-release tablets in pediatric patients.
Gender:
Metformin pharmacokinetic parameters did not differ significantly between normal subjects and patients with type 2 diabetes mellitus when analyzed according to gender (males=19, females=16).
Race:
No studies of metformin pharmacokinetic parameters according to race have been performed.
Drug Interactions
In Vivo Assessment of Drug Interactions:
|
Coadministered Drug
|
Dose of Coadministered Drug
|
Dose of
Metformin HCl |
Geometric Mean Ratio
(ratio with/without coadministered drug) No Effect = 1.00 |
||
|
|
AUC
|
Cmax
|
|||
|
No dosing adjustments required for the following:
|
|||||
| Glyburide |
5 mg |
850 mg |
metformin |
0.91
|
0.93
|
| Furosemide |
40 mg |
850 mg |
metformin |
1.09
|
1.22
|
| Nifedipine |
10 mg |
850 mg |
metformin |
1.16 |
1.21 |
| Propranolol |
40 mg |
850 mg |
metformin |
0.90 |
0.94 |
| Ibuprofen |
400 mg |
850 mg |
metformin |
1.05
|
1.07
|
|
Cationic drugs eliminated by renal tubular secretion may reduce metformin elimination [See Warnings and Precautions (5.1) and Drug Interactions (7). ] |
|||||
| Cimetidine |
400 mg |
850 mg |
metformin |
1.40 |
1.61 |
|
Carbonic anhydrase inhibitors may cause metabolic acidosis [See Warnings and Precautions (5.1) and Drug Interactions (7) .] |
|||||
| Topiramate |
100 mg
|
500 mg
|
metformin |
1.25
|
1.17 |
|
Coadministered Drug
|
Dose of Coadministered Drug
|
Dose of Metformin HCl
|
Geometric Mean Ratio
(ratio with/without metformin) No Effect = 1.00 |
||
|
AUC
|
Cmax
|
||||
|
No dosing adjustments required for the following:
|
|||||
| Glyburide |
5 mg |
850 mg |
glyburide |
0.78
|
0.63
|
| Furosemide |
40 mg |
850 mg |
furosemide |
0.87
|
0.69
|
| Nifedipine |
10 mg |
850 mg |
nifedipine |
1.10
|
1.08 |
| Propranolol |
40 mg |
850 mg |
propranolol |
1.01
|
1.02 |
| Ibuprofen |
400 mg |
850 mg |
ibuprofen |
0.97
|
1.01
|
| Cimetidine |
400 mg |
850 mg |
cimetidine |
0.95
|
1.01 |
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term carcinogenicity studies have been performed in rats (dosing duration of 104 weeks) and mice (dosing duration of 91 weeks) at doses up to and including 900 mg/kg/day and 1,500 mg/kg/day, respectively. These doses are both approximately 3 times the maximum recommended human daily dose of 2550 mg based on body surface area comparisons. No evidence of carcinogenicity with metformin was found in either male or female mice. Similarly, there was no tumorigenic potential observed with metformin in male rats. There was, however, an increased incidence of benign stromal uterine polyps in female rats treated with 900 mg/kg/day.
There was no evidence of a mutagenic potential of metforminin the following in vitro tests: Ames test (S. typhimurium), gene mutation test (mouse lymphoma cells), or chromosomal aberrations test (human lymphocytes). Results in the in vivo mouse micronucleus test were also negative.
Fertility of male or female rats was unaffected by metformin when administered at doses as high as 600 mg/kg/day, which is approximately 2 times the maximum recommended human daily dose of 2550 mg based on body surface area comparisons.
14 CLINICAL STUDIES
A 24-week, double-blind, placebo-controlled study of metformin HCl extended-release tablets, taken once daily with the evening meal, was conducted in patients with type 2 diabetes mellitus who had failed to achieve glycemic control with diet and exercise. Patients entering the study had a mean baseline HbA1c of 8.0% and a mean baseline FPG of 176 mg/dL. The treatment dose was increased to 1,500 mg once daily if at Week 12 HbA1c was ≥7.0% but <8.0% (patients with HbA1c ≥8.0% were discontinued from the study). At the final visit (24-week), mean HbA1c had increased 0.2% from baseline in placebo patients and decreased 0.6% with metformin HCl extended-release tablets.
A 16-week, double-blind, placebo-controlled, dose-response study of metformin HCl extended-release tablets, taken once daily with the evening meal or twice daily with meals, was conducted in patients with type 2 diabetes mellitus who had failed to achieve glycemic control with diet and exercise. The results are shown in Table 7.
|
Metformin HCl Extended-Release Tablets
|
Placebo
|
|||||
|
500 mg
Once Daily |
1,000 mg
Once Daily |
1,500 mg
Once Daily |
2,000 mg
Once Daily |
1,000 mg Twice
Daily |
||
|
Hemoglobin A1c (%)
Baseline Change at FINAL VISIT p-valuea |
(n=115)
8.2 –0.4 <0.001 |
(n=115)
8.4 –0.6 <0.001 |
(n=111)
8.3 –0.9 <0.001 |
(n=125)
8.4 –0.8 <0.001 |
(n=112)
8.4 –1.1 <0.001 |
(n=111)
8.4 0.1 – |
|
FPG (mg/dL)
Baseline Change at FINAL VISIT p-valuea |
(n=126)
182.7 –15.2 <0.001 |
(n=118)
183.7 –19.3 <0.001 |
(n=120)
178.9 –28.5 <0.001 |
(n=132)
181.0 –29.9 <0.001 |
(n=122)
181.6 –33.6 <0.001 |
(n=113)
179.6 7.6 – |
aAll comparisons versus Placebo
Mean baseline body weight was 193 lbs, 192 lbs, 188 lbs, 196 lbs, 193 lbs and 194 lbs in the metformin HCl extended-release tablets 500 mg, 1,000 mg, 1,500 mg, and 2,000 mg once daily, 1,000 mg twice daily and placebo arms, respectively. Mean change in body weight from baseline to week 16 was -1.3 lbs, -1.3 lbs, -0.7 lbs, -1.5 lbs, -2.2 lbs and -1.8 lbs, respectively.
A 24-week, double-blind, randomized study of metformin HCl extended-release tablets, taken once daily with the evening meal, and metformin HCl tablets, taken twice daily (with breakfast and evening meal), was conducted in patients with type 2 diabetes mellitus who had been treated with metformin HCl tablets 500 mg twice daily for at least 8 weeks prior to study entry. The results are shown in Table 8.
|
|
Metformin
HCl 500 mg Twice Daily |
Metformin HCl Extended-Release
|
|
|
1,000 mg
Once Daily |
1,500 mg
Once Daily |
||
|
Hemoglobin A1c (%)
Baseline Change at FINAL VISIT (95% CI) |
(n=67)
7.06 0.14a (–0.04, 0.31) |
(n=72)
6.99 0.27 (0.11, 0.43) |
(n=66)
7.02 0.13 (–0.02, 0.28) |
|
FPG (mg/dL)
Baseline Change at FINAL VISIT (95% CI) |
(n=69)
127.2 14.0 |
(n=72)
131.0 11.5 (4.4, 18.6) |
(n=70)
131.4 7.6 (1.0, 14.2) |
| (7.0, 21.0) |
†a n=68
Mean baseline body weight was 210 lbs, 203 lbs and 193 lbs in the metformin HCl tablets 500 mg twice daily, and metformin HCl extended-release tablets 1,000 mg and 1,500 mg once daily arms, respectively. Mean change in body weight from baseline to week 24 was 0.9 lbs, 1.1 lbs and 0.9 lbs, respectively.